Peer-reviewed CPD content written by pharmacists and clinical experts – free for all healthcare professionals.
- Hundreds of modules to choose from
- Different formats to suit your learning style including podcasts and quick to complete quizzes
- Certificate to validate your learning
- Log sheets and a unique learning record to aid your revalidation submissions
All available for free on the C+D Community – start browsing today

I’ve become an independent prescriber. So, what’s next?
Taking a minor illness course helped Gurinder Singh take his career to the next level. But once it was completed, which doors did it open?

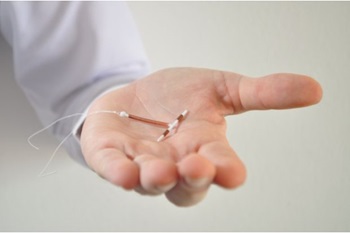
Can this individuals vasectomy be successfully reversed
A patient is worried she will never be able to have children with her partner due to his recent vasectomy

What causes erectile dysfunction
Erectile dysfunction is very common, affecting around 50% of men aged 40-70 years at least once with prevalence and severity increasing with age. Despite these figures, it is not a normal part of the ageing process and there are many reasons why erectile dysfunction can occur, including physical, psychological and drug-related issues. Erectile dysfunction is a symptom and not a disease, and it is therefore important to identify any underlying disease or condition that may be causing it.

Maintaining a healthy diet during pregnancy
Healthy eating and keeping physically active during pregnancy is recommended for women to stay healthy and to prevent excessive weight gain. A healthy diet is particularly important during pregnancy to support the health of both mother and baby. Pregnant women do not need to go on a special diet but should be reminded it is important to eat a variety of different foods every day to get the right balance of nutrients for themselves and their baby.
Chronic obstructive pulmonary disease: treatment and management
COPD treatment is aimed at preventing and controlling symptoms, but do you know the stepwise approach?

Does this COPD exacerbation require antibiotic therapy
Was this patient’s GP correct to send them home with inhaler advice alone?
Female infertility prevalence and management
What do you know about the reasons for female infertility and possible management strategies?

Antimicrobial stewardship in community pharmacy
What do you know about the causes of antimicrobial resistance and your role in fighting it?

Intramuscular injection technique: refresher for pharmacists
From flu vaccines to travel health services, and now COVID vaccinations, injections are becoming part of the daily routine in community pharmacy. Is your technique up to scratch?

Are you missing undiagnosed cases of COPD
Why are cases of COPD not being identified, and what can community pharmacists do about it?
Vitamin deficiency: fat-soluble vitamins
Do you understand the benefits and risks associated with vitamin supplementation and the consequences of deficiencies in fat-soluble vitamins?
You must sign in to use this functionality
Learning
Learning
Authentication.SignIn.HeadSignInHeader
Learning
Learning
Email Article
All set! This article has been sent to my@email.address.
All fields are required. For multiple recipients, separate email addresses with a semicolon.
Please Note: Only individuals with an active subscription will be able to access the full article. All other readers will be directed to the abstract and would need to subscribe.