Offering support to patients with bladder weakness
Download the Offering support to patients with bladder weakness poster here.
What is bladder weakness?
Bladder weakness, also known as incontinence, is when urine leaks from the bladder involuntarily.(1) In urinary incontinence, the process of storing and passing urine is disrupted.(1) It is a problem that a lot of people feel uncomfortable talking about and this stigma often stops many of them from seeking advice.(2)
Prevalence of bladder weakness
In the UK it is estimated that between 3 and 6 million people experience some degree of urinary incontinence.(2) It is a condition that affects both men and women, but tends to be more prevalent in women and is also more common with increasing age.(2,3) The degree and severity of urinary incontinence varies from person to person.(1)
Types of bladder weakness
The process of passing urine is regulated by the sphincter muscles and pelvic floor muscles.(4) There are several types of urinary incontinence but the most common are stress incontinence and urge incontinence.(1)
Stress incontinence
Urine leakage occurs due to extra pressure on the bladder, for example during activities such as coughing, laughing, sneezing or exercising. This is the most common form of incontinence in women and often happens during pregnancy, after childbirth and menopause due to damage to, or weakening of, the pelvic floor muscles and ligaments or if the urethral sphincter is damaged.(1)
Neurological conditions such as Parkinson’s disease and multiple sclerosis may cause damage to these muscles, resulting in stress incontinence. Chronic constipation, obesity and some connective tissue disorders can cause stress incontinence.(1)
Urge incontinence
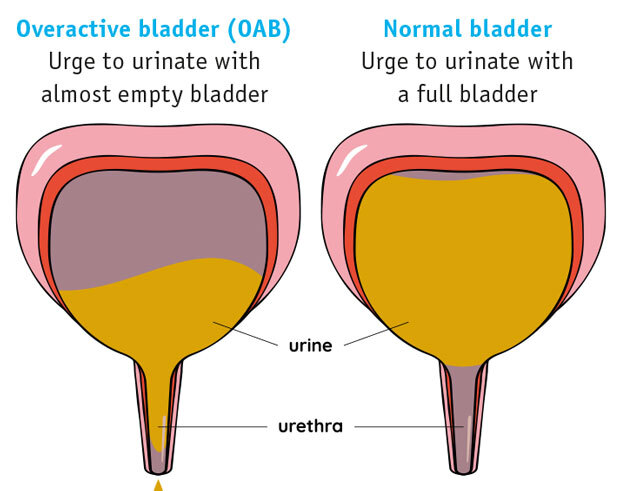
The detrusor muscles, which relax when the bladder fills with urine, can sometimes contract involuntarily, creating an urgent need to go to the toilet. This is known as an overactive bladder (OAB).(5) OAB can increase the frequency of needing to pass urine – the need to urinate during the night is common.(2)
Conditions such as stroke, Parkinson’s disease and urinary tract infections, can cause these symptoms. While some people think reducing fluid intake will help relieve symptoms, it generally makes them worse because concentrated urine can aggravate the bladder.(1)
Other types of urinary incontinence
Less common forms of bladder weakness include:(1,2)
- Mixed incontinence – Symptoms of both stress and urge incontinence.
- Overflow incontinence – The bladder cannot completely empty when passing urine. This may be due to a blockage or obstruction of the bladder or to muscle or nerve damage. Leaks are also frequent.
- Total incontinence – A severe condition in which the bladder cannot store any urine, causing constant passage of large amounts of urine, even at night, or passing large amounts of urine occasionally, with small leaks in between.
Treatment
Conservative treatments such as pelvic floor exercises (Kegel exercises), lifestyle changes and bladder training are often preferred first line for urinary incontinence. Physiotherapy can also be recommended.(1)
Patients can be advised on the following lifestyle changes to improve symptoms:(1,6)
- Reduce caffeine intake
- Alter fluid intake
- Lose weight if overweight or obese
- Stop smoking because coughing puts strain on pelvic floor muscles
- Avoid heavy lifting, which can put pressure on pelvic floor muscles
- Reduce alcohol intake
- Avoid spicy and acidic foods that may irritate the bladder
- Underlying conditions should be treated alongside incontinence.(1)
Pelvic floor exercises
Research has shown pelvic floor exercises, performed several times a day, can benefit everyone with urinary incontinence.(1) Pelvic floor exercises, which involve squeezing the muscles at the front and back of the pelvic floor, will strengthen the muscles around the bladder and help to prevent any leaks.(7)
The pharmacy team is ideally placed to give patients advice on exercises, including providing leaflets and signposting to resources for pelvic floor exercises.
Bladder training
Bladder training can help to improve the symptoms of OAB by focusing on increasing the amount of urine the bladder can hold and reducing the frequency of urination.
Bladder training techniques aim to reduce the amount of times needed to pass urine in 24 hours and involve gradually lengthening the time between feeling the need to urinate and passing urine.(1,4)
Understanding customers with incontinence
While some people are quick to accept their bladder condition, many avoid talking about it altogether. By understanding what these customers need, you can start a conversation that could result in improving their quality of life.
References
- NHS (2019) Urinary incontinence
- NHS Inform (2020) Urinary incontinence
- Mayo Clinic (2019) Urinary incontinence
- Guys and St Thomas’ NHS Foundation Trust (2020) Bladder retraining – treatment for urgency and urge incontinence
- Srikrishna S, Robinson D, Cardozo L, Vella M. Management of overactive bladder syndrome. Postgrad Med J. 2007;83(981):481-486. doi:10.1136/pgmj.2007.057232
- NHS (2019) 10 ways to stop leaks
- NHS (2020) What are pelvic floor exercises?